Lipase Levels Charts: Normal & High Levels in Pancreatitis & Others.
Our content is not intended nor recommended as a substitute for medical advice by your doctor. Use for informational purposes only.
Lipase is a famous lab test that is widely used as a test for acute pancreatitis.
Today, you will learn about various levels (with charts) and possible causes.
1. What is lipase?
Lipase is a small protein molecule that helps your body digest fats (a digestive enzyme). It is produced mainly by the pancreas to digest the fats you eat.
The enzyme is produced by specialized cells in the pancreas. Then, it is transported to the digestive tract (the duodenum) through the pancreatic duct.
Normally, a small trace of the lipase enzyme is detectable in your blood. When the pancreas inflames, large amounts of lipase leak into your blood, leading to elevated lipase levels.
However, lipase is also present in other sites of your body (in lesser amounts).
Other body tissues that have lipase are:
- Salivary glands.
- The gastrointestinal tract (The intestine, the colon, the liver, and the gallbladder).
- Female reproductive system (the ovaries, uterus, and fallopian tubes).
- Tumor tissues (particularly ovarian, prostate, lung, esophageal, and breast cancers). Also, in multiple myeloma and suprarenal gland tumors.
- The brain.
2. Normal lipase levels chart.
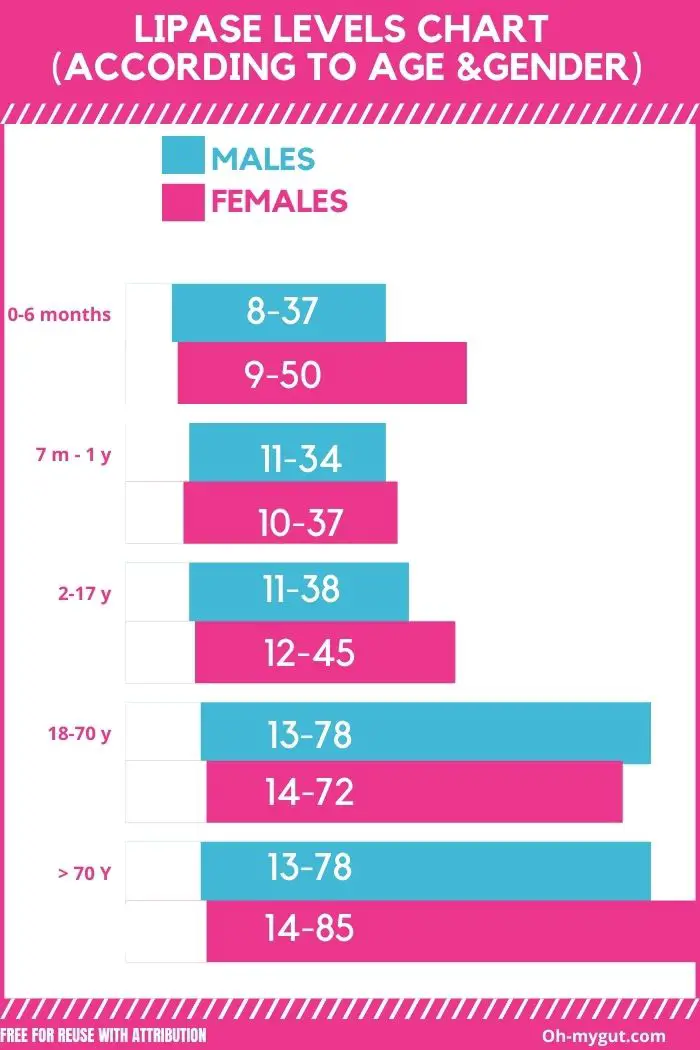
The normal lipase levels in adults range from about 13 up to 78. There are slight differences in cut-off levels for age and gender.
The chart below illustrates the normal lipase levels for males and females according to age.
The numbers below are from the famous U.S. Lab (LabCorp®). Normal levels often vary among different laboratories and centers.
Also, you must note that slight elevations in lipase levels don’t mean you have pancreatitis.
For acute pancreatitis to be diagnosed, the elevation in serum lipase should exceed three times the upper limit of normal. Moreover, you should also have either typical pancreatic pain or evidence of pancreatitis in abdominal imaging.
Slight elevations in serum lipase are often due to causes other than pancreatitis, such as liver diseases, salivary gland diseases, alcoholism, kidney disease, medications, etc.
The table in the next section mentions the full list of causes of elevated lipase.
Moreover, an asymptomatic mild increase in serum lipase is often not a thing to be extremely worried about. Your doctor may or may not require investigations.
Literature refers to asymptomatic elevations in serum lipase without evidence of pancreatic diseases (Gullo’s syndrome) or (benign pancreatic hyperenzymemia).
3. Lipase levels chart and meaning in pancreatitis.
Lipase is one of the most widely used tests to diagnose pancreatitis. Patients with elevated lipase levels (usually above 1000) are most likely to have pancreatitis until proven otherwise.
The common cut-off lipase levels for acute pancreatitis diagnosis is three times or more than the upper limit of normal.
The three times upper limit of normal for adults above 18 years old are:
- For Males: 78 U/L X 3 = 234 U/L
- For Females: 72 U/L X 3 = 216 U/L.
Note that the upper limits are different among different laboratories and health centers. We used the cut-off levels used by the famous laboratory LabCorp®.
Lipase is better than amylase in diagnosing acute pancreatitis because it becomes elevated early and remains so for 8-14 days on average (reference).
On the other hand, amylase remains elevated only for 2-3 days after the onset of pancreatitis. So, it may miss people with late presentation of acute pancreatitis.
Is lipase 100% specific for acute pancreatitis?
As we explained before, lipase is found in various sites in your body other than the pancreas. Although a practical test for pancreatitis, It is not 100% specific for pancreatitis.
Here are some facts from the research:
- Up to 13% of patients with non-pancreatic abdominal pain have elevated lipase.
- Up to 24% of patients with diabetic ketoacidosis (DKA) have elevated lipase (and abdominal pain).
- And many other causes (see the next section) can cause elevated lipase levels without pancreatitis.
- Also, the absence of elevated lipase doesn’t completely exclude acute pancreatitis (especially in recurrent cases.
And that’s why we don’t depend on serum lipase as the sole diagnostic test for acute pancreatitis.
So, what is the scientific way to diagnose acute pancreatitis?
To avoid the cause of elevated lipase (other than pancreatitis), the guidelines recommend diagnosing acute pancreatitis based on the presence of two out of three of the following (reference):
- Elevated serum lipase is more than three times the upper limit of normal (3X ULN).
- Typical pancreatic pain: acute onset, severe, persistent pain in the epigastric area (upper central abdomen). The pain often radiates to the back.
- Characteristic findings of pancreatitis in abdominal imaging (by contrast-enhanced CT, MRI, or abdominal ultrasonography).
So, lipase is not taken alone as a diagnosis of pancreatitis. Your doctor must combine its result with at least one of the two other diagnostic criteria (the pain and imaging of the abdomen).
Moreover, acute onset of typical pancreatic pain and characterizing findings of pancreatitis in abdominal imaging diagnoses pancreatitis without the need for serum lipase to be elevated.
How long does it take for lipase to go down in acute pancreatitis?
In acute pancreatitis, lipase typically remains elevated for more than a week. Then, it starts to go down after an average of 8-14 days. The levels of lipase don’t reflect the severity of pancreatitis.
On the other hand, amylase levels start to go down rapidly after 48-72 hours of the initial rise. Therefore, patients with late presentation of acute pancreatitis may show normal or only slightly elevated amylase.
So, lipase is generally preferred over amylase in assessing acute pancreatitis.
4. What are other causes of high lipase levels?
Several causes of elevated lipase enzyme (other than pancreatitis) are identified.
Elevated serum lipase (particularly when the elevation is mild) can be due to problems elsewhere in other body organs where lipase is located (such as the stomach, intestines, the liver, the gallbladder, and the salivary glands).
Also, many medications may affect the levels of lipase.
The tables below illustrate the diseases (Table 1) and medications (Table 2) that cause elevations in serum lipase (reference).
Table1: Causes of elevated serum lipase.
| Acute pancreatitis |
| Chronic pancreatitis |
| Renal failure |
| Acute cholecystitis |
| Bowel obstruction or infarction |
| Duodenal ulceration |
| Pancreatic calculus |
| Pancreatic tumors |
| Type 2 diabetes mellitus |
| Diabetic ketoacidosis |
| HIV disease |
| HCV infection |
| Macrolipasemia |
| Post-ERCP/trauma |
| Sarcoidosis |
| Celiac disease |
| Inflammatory bowel disease |
| Idiopathic |
| Drugs |
Table 2: Drugs that increase serum lipase levels:
Drugs Causing Elevated Lipase |
| Adrenocorticotropic hormone |
| Ardeparin |
| Cholinergics (eg, bethanechol) |
| Dipeptidyl peptidase-4 (DPP-4) inhibitors |
| Fat emulsions |
| Furosemide |
| Indomethacin |
| Methacholine |
| Methylprednisolone |
| Metronidazole |
| Narcotics (eg, codeine) |
| Oral contraceptives |
| Pegaspargase |
| Pentazocine |
| Secretin |
| Sulfisoxazole |
| Thiazide diuretics |
| Triprolidine/pseudoephedrine |
| Valproic acid |
| Zalcitabine |
Related: What causes a slightly elevated lipase?
5. What levels of lipase are fatal?
The average lipase levels during acute pancreatitis are between 1000 and 10,000 UL. Their magnitude of elevation of serum lipase is not correlated to the severity of pancreatitis. So, there are no specific levels of lipase above which pancreatitis is fatal.
A patient may die with lipase levels below 1000, while another one may survive acute pancreatitis without complications with lipase levels > 10,000 U/L.
So, How do we know if pancreatitis is severe or fatal?
To determine pancreatitis’s severity (or mortality risk), doctors often use a combination of laboratory and clinical indicators that correlate with the severity.
Researchers developed several scores to assess the severity/fatality of pancreatitis. The most famous score is called Ranson’s criteria.
Interestingly, Serum lipase is not among the criteria of severe acute pancreatitis as it poorly correlates with the severity of the disease.
Ranson’s criteria depend on a set of parameters that correlates with the severity of pancreatitis (Reference):
- Age (older than 55 are considered at higher risk of severe/fatal pancreatitis).
- Higher WBCs (white blood cell count).
- Elevations in blood glucose levels.
- An elevated Liver enzyme (AST).
- LDH (lactate Dehydrogenase) level.
- Decrease in Hematocrit.
- Elevated BUN (blood urea nitrogen).
- Decrease in Serum calcium.
- Decrease in Oxygen (PaO2).
- Base defect (acidosis).
- Degree of dehydration (fluid sequestration).
These parameters correlate with the severity and the likelihood of complications and mortality in patients with acute pancreatitis.
The more criteria you have, The higher the risk of complications and death from acute pancreatitis.
- Evidence-based
- Written by a doctor.

















