Best and Worst Sugars for IBS: GI doctor Explains.
Our content is not intended nor recommended as a substitute for medical advice by your doctor. Use for informational purposes only.
This article delves into the realm of sugars and their impact on Irritable Bowel Syndrome (IBS).
Drawing upon the expertise of a GI doctor, we outline the best and worst types of sugars for those managing IBS, emphasizing their FODMAP content.
FODMAPs, or Fermentable Oligosaccharides, Disaccharides, Monosaccharides, and Polyols, are specific types of carbohydrates that can exacerbate IBS symptoms. Understanding which sugars can aid or hinder your control over IBS can be crucial in managing this complex condition.
Let’s take a look at the good and bad sugars for IBS:
| Good Sugars (Low-FODMAP) | Bad Sugars (High-FODMAP) |
|---|---|
| 1. White Sugar (Table Sugar or Sucrose) | 1. Fructose (predominant sugar in most fruits) |
| 2. Brown Sugar | 2. Lactose |
| 3. Glucose | 3. Sorbitol |
| 4. Raw Sugar | 4. Xylitol |
| 5. Stevia | 5. Mannitol |
| 6. Aspartame | 6. Honey |
| 7. Saccharin | 7. High-fructose corn syrup |
| 8. Acesulfame K | 8. Agave syrup |
| 9. Maple Syrup | 9. Isomalt |
| 10. Sucralose | |
| 11. Erythritol |
Please note that these lists represent a general guideline, and individual responses can vary. The ‘best’ sugars are those considered low in FODMAPs and less likely to trigger IBS symptoms.
However, consuming these sugars in moderation is still advised. The ‘worst’ sugars are high in FODMAPs and more likely to trigger IBS symptoms.
Best Sugars for IBS (Low-FODMAP):
Several sugar types are considered ‘IBS-friendly’ due to their low FODMAP content. Here is a breakdown of some of these sugars, their sources, and why they are less likely to trigger IBS symptoms.
1. White Sugar (Table Sugar or Sucrose):
White sugar, or table sugar or sucrose, is derived from sugarcane or sugar beets. It’s a low-FODMAP sugar, making it easier for your body to digest and less likely to trigger IBS symptoms. Sucrose is used in sweet foods like cakes, cookies, and candies. Remember that while it’s a safer choice for people with IBS, consuming it excessively can lead to other health issues.
But Note: This 2019 study suggests that reducing Starch and Sucrose in diet improved IBS symptoms in 50% of patients. So, Table sugar is not 100% safe for all people with IBS. Keeping a food diary and working with a dietitian is a must if you suspect white sugar is triggering your IBS.

2. Brown Sugar:
Brown sugar’s white sugar with a twist – it’s mixed with molasses, which gives it that darker color and a bit more pizzazz in the flavor department. It’s another low-FODMAP friend for those with IBS, and it’s pretty good in recipes where you’d normally use white sugar. Baked goodies like gingerbread and apple pie? They love a bit of brown sugar.
3. Glucose:
Glucose is a simple sugar in various fruits, vegetables, and honey. Even though it’s often found chilling with other types of sugars, glucose itself is low in FODMAPs, making it a cool friend for your IBS. You can get glucose directly from fruits or sweeteners based on it.
4. Raw Sugar:
Raw sugar, like brown sugar, is a less processed version of white sugar and holds onto that molasses flavor. This low-FODMAP sugar option can fill in for brown and white sugars in your recipes. But remember, all sugars – even the good guys – should be consumed in moderation.
5. Stevia:
Straight from the leaves of the Stevia rebaudiana plant comes Stevia, a natural sweetener. It’s got zero calories and is low in FODMAPs, which makes it an excellent choice for people with IBS. You can use it in drinks, cereals, and baked goods.
6. Aspartame:
Aspartame is an artificial sweetener that doesn’t bring a ton of calories to the party. You’ll find it in many diet drinks and sugar-free goodies. It’s low in FODMAPs, making it a solid sugar substitute for IBS folks. Still, be careful – some people might be sensitive to aspartame.
7. Saccharin:
Meet Saccharin, another low-calorie artificial sweetener. It’s the star of many diet products, sugar-free candies, and medicines. Saccharin is low in FODMAPs, so it’s another good sugar substitute for IBS sufferers. It has a long history of use, though some people don’t like its slightly metallic aftertaste.
8. Acesulfame K:
Acesulfame K, also known as acesulfame potassium, is a super sweet, calorie-free sugar substitute. It’s low in FODMAPs, so it’s a safe bet for people with IBS. You’ll often find it paired up with other sweeteners in processed foods.
9. Maple Syrup:
Ah, maple syrup – this natural sweetener, hailing from the sap of maple trees, is low in FODMAPs and a favorite for pancakes, waffles, and all kinds of desserts. It’s a better choice for those with IBS, but remember, it’s still sugar-laden, so a little goes a long way.
10. Sucralose:
Under the brand name Splenda, you’ll find sucralose, a zero-calorie artificial sweetener. It’s low in FODMAPs and common in diet drinks and sugar-free products. It’s usually safe for most IBS folks, but some find it triggers symptoms, so use it wisely.
11. Erythritol:
Erythritol is a sugar alcohol found naturally in some fruits and fermented foods. It’s low-calorie and doesn’t mess with your blood sugar levels like regular sugar. Being a low-FODMAP sugar substitute, it’s typically well-tolerated by IBS peeps. You can use erythritol in baking and cooking.
Due to their low FODMAP content, these sugars and sweeteners can be part of an IBS-friendly diet. However, as with all foods, they should be consumed in moderation. What works for one person may not work for another, so monitoring your symptoms and making dietary adjustments as needed is crucial. Always consult with a dietitian or healthcare professional before making significant changes to your diet.
Bad sugars for IBS (high-FODMAP)
1. Fructose (predominant sugar in most fruits):
Fructose, a monosaccharide sugar, is plentiful in most fruits, honey, and numerous processed food items. Although it’s a naturally occurring sugar and typically part of a balanced diet, it can lead to digestive problems in individuals with IBS due to its high-FODMAP characteristics.
Let’s examine fructose in greater depth:
- Where it comes from: Fruits such as apples, pears, mangos, and watermelons are high in fructose. Moreover, fructose is a key component in honey and high-fructose corn syrup, a common ingredient in many processed foods.
- FODMAP content: When fructose is consumed in quantities exceeding glucose, it is categorized as a high-FODMAP sugar. This is frequently the case in fruits, honey, and foods sweetened with high-fructose corn syrup.
- Implications for IBS: Some people struggle to absorb fructose, leading to fermentation in the gut. This process can trigger bloating, gas, and diarrhea – typical symptoms of IBS. Those with IBS are potentially more susceptible to fructose intolerance.
2. Lactose:
Lactose is a disaccharide sugar present in milk and dairy products. It’s notorious for causing digestive difficulties in people who are lactose intolerant, but it’s also a high-FODMAP sugar, which can cause discomfort in individuals with IBS.
Here’s a deeper dive into lactose:
- Where it comes from: Primarily, lactose is found in milk and dairy products such as cheese, butter, and yogurt. Moreover, it’s frequently added to processed foods, making label reading crucial.
- FODMAP content: Lactose is classified as a high-FODMAP food. Fermentable oligosaccharides, disaccharides, monosaccharides, and polyols (FODMAPs) are carbohydrates that are often challenging to digest and may induce IBS symptoms.
- Why It’s Bad for IBS: In the gut, undigested lactose can cause water to be drawn into the intestines, resulting in diarrhea. Additionally, when bacteria in the gut ferment it, it can cause bloating and gas, symptoms often experienced by individuals with IBS.
3. Sorbitol:
Sorbitol is a sugar alcohol. It is commonly found in fruits like apples, pears, and peaches and is often used as a sweetener in sugar-free products. We consider sorbitol a high-FODMAP food and can cause digestive issues for individuals with IBS, including gas, bloating, and diarrhea.
4. Xylitol:
Xylitol, another sugar alcohol, is often found in sugar-free gums, candies, and some medications. Despite being low in calories, xylitol is a high-FODMAP food and can cause significant digestive distress in those with IBS, leading to symptoms like bloating, gas, and diarrhea.
5. Mannitol:
Mannitol is a sugar alcohol found in some fruits and vegetables, and it’s also used as a sweetener in various sugar-free products. Like sorbitol and xylitol, mannitol is a high-FODMAP food that can exacerbate IBS symptoms.
6. Honey:
Although honey is frequently chosen as a natural and healthier sweetener substitute for table sugar, those with Irritable Bowel Syndrome (IBS) must be cautious. The substantial fructose levels in honey categorize it as a high-FODMAP food, potentially provoking IBS symptoms.
Let’s examine honey more closely:
- Where it comes from: It is produced by bees, and honey is a commonly used sweetener in many foods and beverages, including tea and baked goods.
- FODMAP content: Honey is classified as a high-FODMAP food due to its significant fructose levels. Even minor quantities can trigger the onset of IBS symptoms in susceptible people.
- Its impact on IBS: The high levels of fructose in honey can disrupt the digestive system’s normal function. Like the fructose found in fruits, honey’s fructose can ferment within the gut, leading to symptoms such as bloating, gas, and diarrhea. Consequently, those with IBS are frequently advised to restrict or entirely avoid honey consumption.
7. High-fructose corn syrup:
High-fructose corn syrup is a common sweetener in processed foods and drinks. As the name suggests, it’s high in fructose, making it a high-FODMAP sugar that can cause digestive issues for those with IBS. Avoiding products that contain high-fructose corn syrup can be beneficial for managing IBS symptoms.
8. Agave syrup:
Agave syrup, or agave nectar, is a sweetener from the agave plant. It’s often marketed as a healthier alternative to regular sugar but is high in fructose and thus high in FODMAPs. Consuming agave syrup can trigger symptoms like bloating, gas, and diarrhea for individuals with IBS.
9. Isomalt:
Isomalt is a sugar alcohol commonly used in sugar-free candies and snacks. Like other sugar alcohols, it’s considered a high-FODMAP food and can trigger IBS symptoms. Those with IBS should avoid foods containing isomalt.
These sugars and sweeteners are considered high-FODMAP foods that can trigger IBS symptoms in susceptible individuals. Remember that everyone is unique, and what causes a reaction in one person may not have the same effect on another. If you have IBS and are struggling to manage your symptoms, consider consulting with a dietitian or other healthcare professional specializing in gastrointestinal health. They can provide personalized advice and guidance on adjusting your diet to manage your symptoms best.
Other tips for consuming sugar safely with IBS:
1. Practice Mindful Consumption:
The adage “less is more” is particularly valid regarding sugar intake for IBS sufferers. Consuming excessive quantities of sugar, regardless of its FODMAP status, could instigate IBS symptoms. Hence, maintaining a balanced dietary regimen and careful sugar intake is pivotal in controlling IBS symptoms.
2. Multi-sugar Foods – Pay Attention:
Numerous foods, for example, honey and various fruits, consist of multiple sugar types. To illustrate, honey contains fructose and glucose, while fruits may comprise fructose, glucose, and sucrose. When regulating your sugar intake, it’s critical to consider all sugars present in the food, as some may have a higher FODMAP content than others.
Here is an example of different sugar types present in honey (reference):
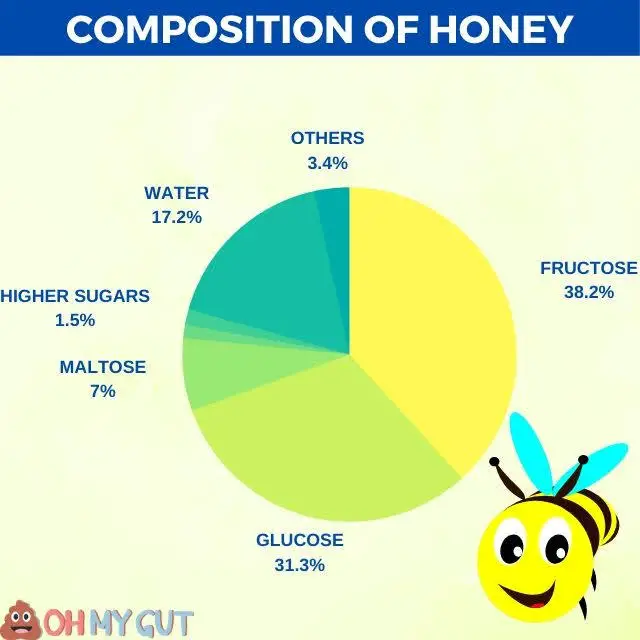
3. Record your Meals:
The best way to deal with an IBS diet mess is to record your meals, also known as a food diary, which can be a practical method to single out specific IBS symptom triggers.
You can discover trends over time by tracking your meals and any subsequent symptoms. This diary can aid in managing your IBS and furnish crucial information for your healthcare provider.
4. FODMAP Content – Keep it Close:
It can be beneficial to have quick access to the FODMAP content of different foods if you’re dealing with IBS.
Multiple apps and online platforms provide this information at your fingertips. Some of these resources even offer the convenience of sorting foods based on their FODMAP content, simplifying meal planning according to your dietary preferences.
The best FODMAP app is Monash University FODMAP app (available for both Android and iPhone), it is a one-time purchase but a life-saver for people with IBS.
Always remember that these suggestions are meant to aid you but should differ from professional medical counsel. If you need more clarification about your diet’s impact on your IBS, always seek advice from a healthcare professional or dietitian. They can provide tailored guidance based on your unique situation and assist in unraveling the intricacies of managing IBS.
FAQS:
1. Does sugar makes IBS worse?
The answer here could be clearer. Not all sugars will upset your IBS, but some might. For instance, fructose (found mostly in fruit), lactose (in dairy), and certain sugar alcohols can be problematic. So, it’s not about avoiding all sugar but more about being mindful of the type and amount you consume.
2. Does cutting out sugar help IBS?
Getting rid of certain sugars, like those high-FODMAP ones I just mentioned, could help calm your IBS. But remember, everyone’s different. Cutting back on sugar does the trick for some folks, while others don’t see much change. It’s always a good idea to check in with your doctor or dietitian about these things – they can help you figure out a game plan that suits you best.
3. White sugar or brown sugar, which is better for IBS?
Both of these are generally okay for people with IBS. They’re both low FODMAP, which means they’re less likely to cause problems. But like all good things, moderation is key – consuming too much sugar can make you feel icky.
4. Is coconut sugar good or bad for IBS?
Coconut sugar is typically fine for IBS sufferers – it’s low-FODMAP, like white and brown sugar. But remember, everyone’s unique, and what works well for one person might not for another. If you notice it triggers your symptoms, it’s best to avoid it. And as always, don’t forget about moderation.
5. Are artificial sweeteners good or bad for IBS?
Some artificial sweeteners are low-FODMAP, making them a decent sugar alternative for folks with IBS. We’re talking about aspartame, Saccharin, acesulfame K, and sucralose. But remember, everyone’s different, and some people might find certain artificial sweeteners still trigger their IBS. Listen to your body; chat with your healthcare provider if you have any doubts or concerns.
- Evidence-based
- Written by a doctor.






