Why do I always have diarrhea? (Doctor Explains)
Our content is not intended nor recommended as a substitute for medical advice by your doctor. Use for informational purposes only.
Hello Everyone. As a gastroenterologist, I get this question almost on a daily basis: Doctor, Why Do I have diarrhea every day?
In fact, Diarrhea is a very common symptom. And from my own experience, People use the term ‘diarrhea every day’ to refer to chronic or recurrent (intermittent) attacks of diarrhea that come and go and usually are not as severe as gastroenteritis.
Today, I will take you on a journey to understand the common causes of such a condition.
Summary: the most common reasons why you always have diarrhea (chronic, for more than one month):
- Lactose intolerance.
- Other forms of food intolerance and allergy, such as fructose and FODMAP intolerance.
- Irritable bowel syndrome with diarrhea.
- Celiac disease.
- Inflammatory bowel disease.
- Bile acid diarrhea.
- Chronic gastrointestinal infections.
- Medications such as proton pump inhibitors, antacids, laxatives, etc.
- Colorectal cancer.
- Other less frequent causes, such as SIBO, lymphoma, hyperthyroidism, etc.
1. Lactose intolerance
Food intolerance is difficulty digesting particular foods, leading to symptoms such as diarrhea, gas, and/or abdominal pain.
The most widespread type of food intolerance is the inability to digest lactose.
How common is lactose intolerance?
Lactose is the primary sugar in milk and dairy products (ice cream, yogurt, cheese, etc.).
Surprisingly, about two-thirds (about 65%) of the world population develop lactose intolerance as they become adults.
Why is it so common?
Lactose intolerance is often a result of the enzyme (lactase) responsible for the breakdown and digestion of lactose.
Most people lose their natural lactose enzymes in the intestine by becoming adults. A phenomenon called (developmental lactose intolerance).
Lactose intolerance is extremely high among certain races, such as African Americans, Hispanics, and Asians.
Symptoms:
Lactose intolerance symptoms will occur daily if you consume milk or other dairy products.
The most common symptoms include:
- You will always have diarrhea after you drink or eat dairy.
- Bloating.
- Distension, flatulence.
- Loose poop (often yellowish or pale brown).
- Nausea.
- Stomach pain.
The symptoms of lactose intolerance can range from mild to extreme forms of diarrhea, vomiting, and abdominal pain.
Consider lactose intolerance if you always have diarrhea after consuming milk and dairy products.
Lactose intolerance is commonly associated with multiple symptoms (bloating, nausea, cramps, and diarrhea). However, some cases may present with diarrhea only.
The most common type of lactose intolerance is primary or essential lactose intolerance, which typically develops as you become an adult.
2. Irritable bowel syndrome.
Irritable bowel syndrome affects too many people worldwide. Approximately 10 to 15% of people have IBS (reference).
Surprisingly, Too many people who match the criteria of IBS don’t seek medical advice. Some studies estimated that 60% of people with IBS symptoms don’t know they have the disease! (reference).
IBS has four subtypes according to the predominant symptom. What concerns us today is the diarrhea-predominant IBS. Diarrhea-predominant IBS is one of the most common reasons you always have diarrhea.
Symptoms (how to suspect IBS-diarrhea):
- Abdominal pain: is the fundamental symptom of IBS. IBS sufferers typically experience abdominal pain at least one day per week.
- The symptoms are often continuous at least one day per week for a minimum of 3 months.
- The abdominal pain either improves or worsens after the bowel movement.
- The onset of abdominal pain is associated with diarrhea and loose stool (change in stool form).
- You may always have diarrhea with IBS. However, diarrhea typically comes and goes in attacks (flare-ups).
- Bloating is frequent in people with IBS.
- Intermittent or constant diarrhea.
- Mucus in the stool.
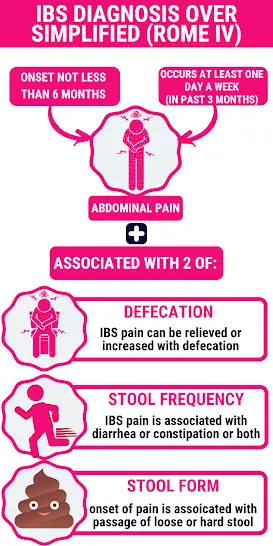
The IBS is usually triggered by:
- Certain foods, such as FODMAPs.
- Alcohol and caffeine.
- Fatty foods and spicy foods.
- Stress and anxiety.
The following symptoms are NOT among IBS symptoms:
- Abdominal pain awakens you at night.
- Fever.
- Blood in stool.
- Weight loss.
- Vomiting.
- Anemia.
IBS is a functional bowel disease. This means we couldn’t find specific lesions by investigation. Therefore, a doctor can only diagnose IBS after excluding other organic diseases.
The ROME IV criteria are the most accepted method for diagnosing IBS. The ROME IV symptom-based criteria. Until now, No specific imaging or lab test can diagnose IBS.
If you suspect IBS is a cause of constant diarrhea. Learn how IBS is diagnosed in this in-depth article.
3. Other forms of food intolerance and allergy.
Intolerance or allergy to certain foods or drinks is a widespread condition. It is estimated that up to 20% of people have some form of food intolerance.
Lactose is a sugar present in milk and other dairy products. Unfortunately, lactose intolerance is shockingly common among some races.
The prevalence of lactose intolerance in the white population is about 20%, which may go up to 90% in certain other races (reference).
Lactose intolerance is just one example of food intolerance. In addition, a long list of foods and drinks can cause food intolerance or allergies.
Common types of food intolerance and allergy:
- Lactose intolerance: In milk, ice cream, mustard, and some types of cheese.
- Fructose intolerance: Present in many fruits and honey.
- FODMAPs intolerance: It affects people with IBS. FODMAPs refer to “Fermentable Oligo-, Di-, Monosaccharides, and Polyols. FODMAPs are a group of short-chain carbohydrates that cause gas and digestive disturbances. They are present in various foods, vegetables, fruits, and artificial sweeteners. Learn more.
- Caffeine intolerance: Caffeine in coffee, teas, and chocolates is one of the most common causes of constant diarrhea. Caffeine is abused in large amounts, raising the risk of diarrhea.
- Alcoholointolerance: Too much alcohol may cause diarrhea; some are high in FODMAPs and can trigger IBS symptoms.
- Gluten intolerance causes Celiac disease (see later) and another milder form called “Non-celiac gluten sensitivity.”
- Amines intolerance: Amines are produced by bacteria during food storage and fermentation.
- Salicylates intolerance: Salicylates are naturally occurring chemicals. They are present in various foods, including fruits, vegetables, coffee, and teas.
- Sulfite intolerance: Sulfite is used as a natural preservative for foods.
- Food allergy: Some foods can cause more severe allergic reactions, such as Nuts, peanuts, raw meat, seafood, mustard, rice, and some fruits and vegetables.
The difference between food intolerances and food allergies is described in the table below:
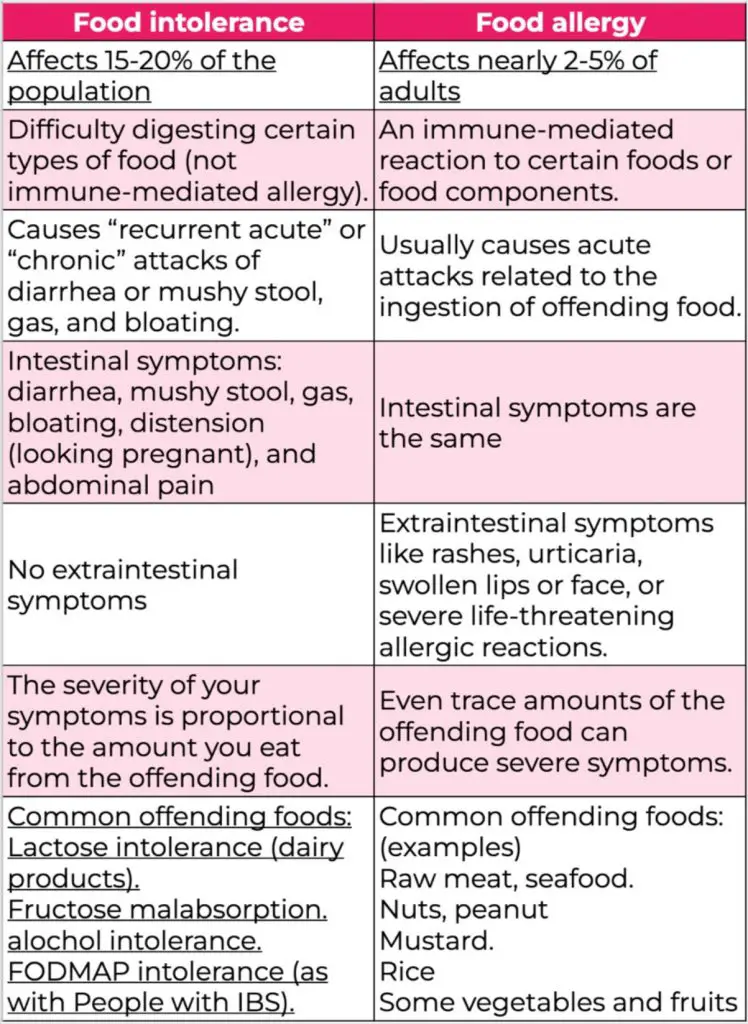
4. Celiac disease
Celiac disease is an extreme form of food intolerance. It is a common disease affecting 1% of the world’s population.
With celiac disease, your body is intolerant to a protein called “gluten.” Gluten is found mainly in:
- Wheat and wheat-based foods such as bread.
- Rye.
- Barley.
A small intestinal inflammation with malabsorption develops after eating gluten-containing foods. Celiac disease can cause constant diarrhea for years if people don’t seek medical advice.
Symptoms suggesting celiac disease:
- The usual age of onset is between 20-30 years of age. But it can occur in older ages up to 70 years.
- Abdominal pain and bloating.
- Constant diarrhea.
- Diarrhea can also be intermittent or not present. Constipation can also occur.
- Nausea and vomiting.
- Weight loss.
- Easy fatigue and iron deficiency anemia.
- Itchy, blistery skin.
- Osteoporosis and osteomalacia (body aches).
Celiac disease is diagnosed by a blood test or taking a small intestine biopsy.
Call your doctor if you suspect celiac disease. Learn more.
5. Inflammatory bowel disease (Crohn’s disease and ulcerative colitis.
Inflammatory bowel disease refers to 2 major conditions:
- Crohn’s disease: Unexplained inflammation and ulceration at any part of your gut (from the mouth to the anus).
- Ulcerative colitis: Unexplained inflammation and ulceration affecting the large intestine only (the colon and the rectum).
According to the CDC, about 1.8 million U.S. adults (0.9%) had inflammatory bowel disease.
Symptoms of IBD:
- Persistent or recurrent diarrhea.
- Abdominal pain.
- Blood or blood and mucus coming out with or without a stool.
- Weight loss.
- Generalized fatigue.
- Fever may occur.
- Loss of appetite.
Suspect IBD if you have a prolonged history of abdominal pain, mucus, constant diarrhea, and blood in stool without obvious cause.
The main differences between Crohn’s and ulcerative colitis are summarized in the below table.
| Type | Crohn’s Disease | Ulcerative Colitis |
|---|---|---|
| 1- Site | Any part of the GI tract (from the mouth to the anus) | The colon and rectum. |
| 2- Lesions | Deeper, it can involve all the layers of the GI wall. | Usually superficial (only in the innermost layer) |
| 3-Predominant symptom | Crampy abdominal pain | Bloody diarrhea. (can be constant) |
| 4- Complications | Fistulas, abscess, intestinal obstruction | hemorrhagic toxic megacolon. |
| 5- Risk of colon cancer | Slight increase | Marked increase |
Ulcerative colitis and Crohn’s disease are major diseases that require medical care and follow-up.
If you have a long history of recurrent abdominal pain, and constant diarrhea with blood, and mucus in stool, consult your doctor.
6. Medications.
Vague constant diarrhea for long periods can result from medications you take. Diarrhea is a documented side effect of more than 700 medications (reference)
Common medications that can cause constant diarrhea:
- Antibiotics: Any antibiotic can kill the beneficial bacteria inside your colon.
- Some anti-diabetes medications: Metformin and gliptins (vildagliptin, sitagliptin, and others), can cause diarrhea and stomach gurgling.
- Laxative overuse.
- Stomach/GERD medications: PPIs (as omeprazole, esomeprazole, and pantoprazole) and H2 blocker inhibit stomach acid. This inhibition will allow for the overgrowth of bacteria inside the small intestine and colon, causing stomach gurgling and diarrhea.
- Others, such as chemotherapy, and immunosuppressive medications, can also cause such conditions.
The complete list of medications causing diarrhea is HERE and HERE.
7. Bile acid diarrhea.
Bile acid diarrhea (BAD) is one of medicine’s most underrated causes of chronic and constant diarrhea.
Normally, your small intestine reabsorbs more than 95% of bile excreted from the liver through the gallbladder and bile duct (reference).
Excess bile acid secretion or malabsorption of the bile acid leads to Bile acid diarrhea.
How common is bile acid diarrhea?
Bile acid diarrhea is more common than you think. And it is often misdiagnosed as IBS-D.
The following facts and statistics will help you imagine the amplitude of BAD:
- About 25 to 50% of patients diagnosed with IBS-diarrhea have BAD (reference.
- It is estimated that about 1% of the population may have BAD.
- It is estimated that about 64% of patients with Functional diarrhea have BAD (reference).
- Up to 35% of people with a condition called “microscopic colitis” have BAD (reference).
Symptoms suggest Bile acid diarrhea.
- Constant diarrhea (especially after fatty meals).
- Extreme urgency: a sudden severe urge to poop.
- Extreme urgency may lead to soiling accidents (stool incontinence) in some people.
- Unlike IBS, diarrhea can occur at night (it awakens you from sleep).
- Abdominal pain and stomach gurgling after meals.
- Bloating and flatulence.
Many doctors overlook bile acid as a cause of always having diarrhea. This is due to the relative unavailability of its specific test (SeHCAT test) and the similarity of symptoms with IBS.
The treatment of bile acid diarrhea is a bile acid binder called cholestyramine (Questran). We discussed the issue of BAD and its relation to IBS-D in-depth HERE.
8. Chronic gut infections.
Recurrent or persistent infections can lead to constant diarrhea. The most common persistent infections that can cause constant diarrhea are (reference):
- Closteroides difficile.
- Aeromonas.
- Giardia.
- Amebae.
- Campylobacter.
- Cryptosporidium.
- Cyclospora.
- Whipple’s disease.
This form of diarrhea is usually severe watery, and constant diarrhea for years. In addition, it may lead to complications such as malabsorption and weight loss.
Chronic infectious diarrhea is more common in people with weak immune systems. Examples are patients receiving chemotherapy, immunosuppressive medications, and people with HIV.
Your doctor usually needs to do a stool culture or take an aspirate from the small intestine or the colon to detect the causative organism.
9. Colorectal cancer.
Abdominal pain alone is a rare presentation of colon cancer. Isolated abdominal pain presents in only 3.8% of colon cancer patients (reference).
A change in bowel habits (such as constant diarrhea) is the most frequent sign of colon cancer.
The recent onset of prolonged constant diarrhea in older ages is suspicious of colorectal cancer, particularly in those with multiple risk factors.
Risk factors for colorectal cancer include:
- Age (especially those who are older than 45 years.
- Family history of colorectal cancer.
- Diet high in fats and processed meats. A low-fiber diet is also a major risk factor.
- Smoking and alcohol abuse.
- Obesity.
- Physical inactivity and sedentary lifestyle.
- Diabetes mellitus.
- IBD.
- African American Race.
Learn more about the risk factors of CRC.
Symptoms of colorectal cancer (with frequency):
- Change in bowel habits (Unexplained diarrhea or constipation): in 75% of patients with colon cancer.
- Blood in the stool (dark or bright red): 50%.
- A sense of rectal mass: in 25%.
- Anemia (iron deficiency): in 10%.
- Isolated abdominal pain: only 3.8% of cases.
- Other symptoms such as weight loss, unexplained fever, nausea, and anorexia are also present.
10. others.
The table below illustrates the causes of chronic diarrhea according to its frequency (reference).

- Evidence-based
- Written by a doctor.