Can GERD Be Cured Permanently? Statistics Reveal The Answer
Quick insights.
- GERD has different types. Not all of them are chronic. So you have to define what type of GERD you have.
- Physiologic GERD (infrequent, related to meals) generally can be controlled or cured. But “clinically significant GERD” is only treatable Not curable in most cases.
- Clinically significant GERD (frequent, nocturnal, or complicated GERD) is usually not cured by diet or lifestyle modification alone.
- Medications are necessary to control and prevent GERD symptoms and complications. But doesn’t provide a permanent cure for the original cause.
- Anti-reflux surgery (if indicated by your doctor) can provide a permanent cure for GERD in a large proportion of people, but it is not for everyone.
The answer depends on what you mean by GERD.
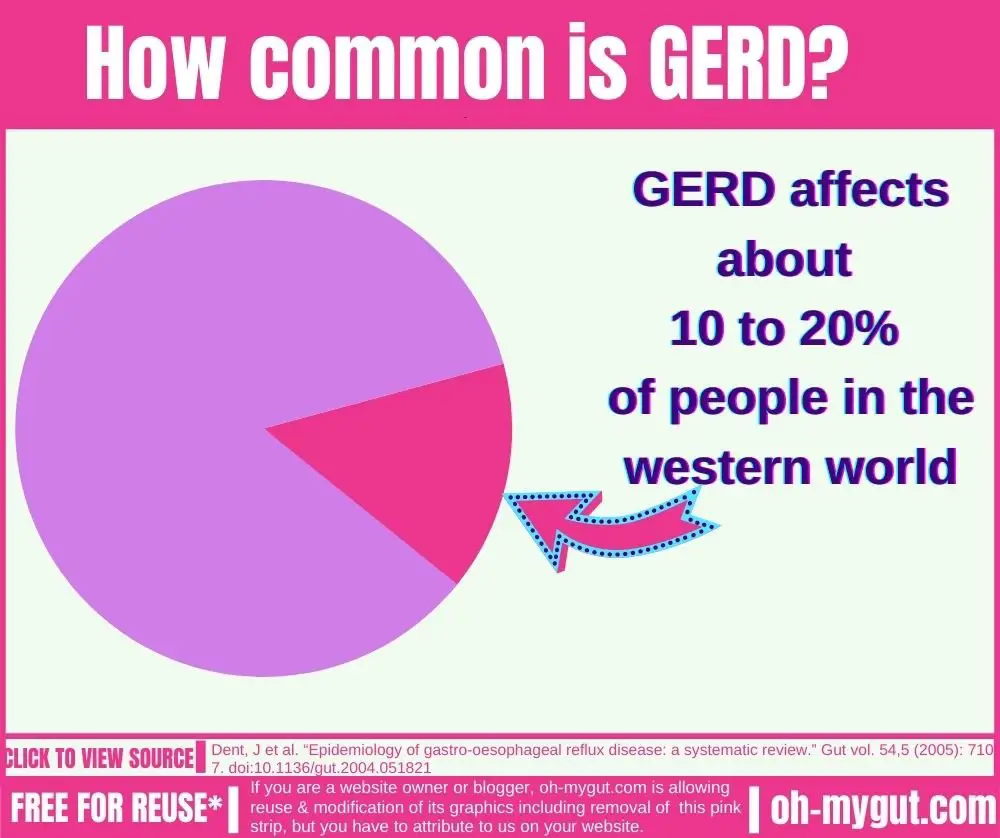
GERD affects about 10 to 20% of people in the western world (ref). In a large USA telephone-based survey (of 21,128 adults), 22% of people reported heartburn or regurgitation during the last month prior to the survey call (ref).
That’s a huge percentage of people who have GERD-like symptoms. This means at least one out of five people has heartburn. And of course, not all of them have chronic, clinically significant GERD.
This is because GERD has different types. Not all of them are chronic. So you have to define what type of GERD you have:
- Physiologic GERD: it usually occurs in normal individuals at a certain point of their life. A tolerable amount of stomach acid is refluxed into the esophagus which will result in mild to moderate symptoms which are: (ref)
- Infrequent, short in duration.
- Often occurs after meals.
- Rarely occurs during sleep time.
- Usually causes NO or mild sporadic acid reflux symptoms (heartburn).
- This type is usually NOT harmful to your esophagus and can be cured with lifestyle and food modifications.
- Clinically significant GERD (affects only 3-6% of people): in this type of GERD heartburn and regurgitation occur more frequently (more than twice/week). The reflux symptoms often occur at night and can be associated with esophageal complications. According to endoscopy, it is further divided into:
- Non Erosive oesophagitis: when you have GERD symptoms, but your doctor cannot detect esophageal damage on performing endoscopy.
- Erosive Oesophagitis: this term means that your doctor detected esophageal inflammation or damage by endoscopy. [sadly, some people can have erosive oesophagitis without symptoms!].
- Physiologic GERD: it usually occurs in normal individuals at a certain point of their life. A tolerable amount of stomach acid is refluxed into the esophagus which will result in mild to moderate symptoms which are: (ref)
- GERD-like conditions:
- Functional Heartburn: it is a type of Functional gut disease where doctors cannot find any evidence of GERD by endoscopy and acid testing. And is usually related to stress and anxiety. Also, it has a poor response to standard treatments such as proton pump inhibitors (PPIs).
- Reflux Hypersensitivity: normal, a physiologic degree of reflux can occur to us and it normally doesn’t result in symptoms. But with certain people, this can result in a special type called “reflux hypersensitivity”.
- Wrong diagnosis: people with other conditions can experience GERD-like symptoms such as eosinophilic esophagitis, achalasia, Bile, reflux, and many others.
These GERD-like symptoms can be identified and cured permanently by your doctor.
Clinically significant GERD is considered a treatable, NOT curable. And to understand what I mean by this, keep reading below.
Generally, GERD is Treatable, Not curable!
Curable means a complete resolution of the diseases “permanently”
While Treatable means disease progression can be slowed, controlled, or even reversed but no complete resolution (ref)
For example, Hypertension is treatable (can be controlled by medications) but it is not curable. While tonsillitis is curable as the disease resolves completely with medications (antibiotics).
Regarding GERD (Acid Reflux), current treatments including lifestyle modification, medications, and surgery successfully control the disease and can reverse the damage. So, GERD is generally considered to be a treatable disease (not curable) (ref). But in certain circumstances, some treatments such as weight loss and surgery can cure your GERD permanently.
In this article, we’ll discuss the clinically significant GERD in which the symptoms are frequent (2 or more per week), occurring at night or GERD with complications such as Barrett’s esophagus.
Can GERD be cured without medications? (only By lifestyle, food, and natural remedies).
Current scientific evidence states that clinically significant GERD (frequent symptoms or presence of complications) cannot be cured by lifestyle or food modification only. Although some were found effective in reducing frequent GERD symptoms, it didn’t provide a complete cure from GERD (ref).
However, if your GERD is infrequent (less than 2 attacks per week) or intermittent (physiologic GERD) lifestyle and food modification may provide a sufficient cure for these mild symptoms.
But what Research tells about the efficacy of different lifestyle & food modifications?
Efficacy of Weight loss:
The single most effective lifestyle modification in improving GERD symptoms is weight loss.
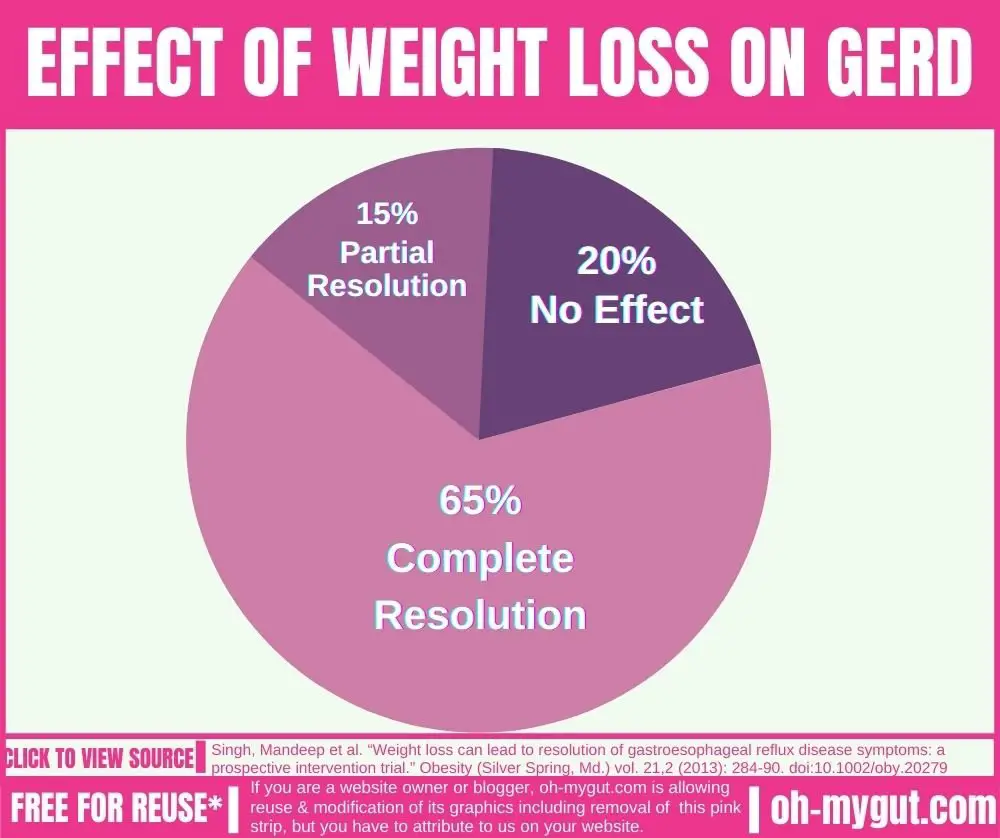
For Example this interesting study, the weight loss resulted in a complete resolution “cure” of GERD symptoms in 65% of persons with GERD (within 6 months). In addition, another 15% experienced partial resolution “improvement” of GERD symptoms with weight loss.
That’s MASSIVE!, a 65% (complete cure) + 15% (partial resolution) = 81% improvement of GERD with weight loss.
So, if you have obesity and GERD, making a decision to lose weight can be a permanent “cure” for your GERD.
Efficacy of smoking cessation, head elevation, and early night meals:
Head elevation consistently improved esophageal acidity and symptoms in research. This leads to partial improvement of the GERD symptoms (not a complete cure) (ref).

WEIGHT LOSS AND HEAD ELEVATIONS ARE CONSIDERED THE 2 MOST EFFECTIVE LIFESTYLE MODIFICATIONS THAT CAN IMPROVE GERD.
Smoking cessation also is considered to be effective in improving GERD symptoms. A large study of 29,610 participants showed that cessation of smoking decreased severe reflux symptoms in non-obese patients who also take GERD medications (ref).
Also, early meals (4-6 hours before bedtime) improved GERD symptoms. (ref).
Can GERD be cured with Diet:
Honestly, the role of food in improving “clinically significant GERD” is limited. Although Avoiding triggers helps to reduce GERD symptoms, this is a partial improvement.
And no food type or food plan can permanently cure severe forms of GERD. (ref).
Food modification can help (not cure) GERD symptoms. And it is NOT routinely recommended for GERD treatment by the American Gastroenterological Association (AGA) Nor the Canadian Association of Gastroenterology) (ref) (ref).
However…
As a long-term strategy, based on a weight-loss dietary program, food can help you lose weight and hence improve your GERD. This is the only strategy that diet can cure your GERD (indirect via weight loss diet plan), but it is only effective if you are obese.
Also, avoiding food triggers can help prevention of worsened GERD symptoms. For example:
- Caffeine.
- High-fat diet.
- Diet low in fiber.
- Chocolate.
- Spicy foods.
- Carbonated beverages.
- Peppermint.
MORE: Don’t Eat Chocolate after Hiatal Hernia Surgery (2 main reasons).
Can GERD Be Cured with Medications?
Several treatments exist that can greatly improve your GERD and Acid reflux Symptoms. Namely:
- Proton Pump inhibitors (PPIs): such as Omeprazole and Esomeprazole.
- H2 Blockers: such as Ranitidine and Famotidine.
- Prokinetic drugs: such as Metoclopramide, Itopride.
- Antacids: such as Sacralfate and Al. Hydroxide.
Proton Pump inhibitors (PPIs) are the most potent acid secretion inhibitors. An 8-week course of PPIs can heal severe GERD and Reverse the esophageal damage caused by acid reflux in 86% of patients with Erosive esophagitis (ref).
But…
Healing of esophageal erosions is not considered a cure. This is because PPIs treat the symptoms and the complications. PPIs have nothing to do with the original causes of GERD such as disordered Lower esophageal Sphincter (LOS) or Hiatal Hernia.
And oesophagitis can occur again after healing as the cause is persistent. And Until this moment, there are no drugs that can directly target the cause of GERD. Also, the long term use of PPIs is linked to some hazards (ref).
And this takes us back to the original principle of the currently available GERD medications. It treats but doesn’t cure GERD. so, it has a great role in preventing the progression of esophageal damage and the prevention of complications such as barrett’s esophagus and esophageal cancer.
And in certain mild cases, when combined with lifestyle and dietary modification can cure your GERD (especially
Work with your doctor to determine the best options for your GERD. There is no black or white answer to your question about “Can GERD be cured?”. The answer always lies in the grey zone depending on multiple factors.
Can surgery cure GERD Permanently?
In selected cases, you may need surgery to control GERD and acid reflux. Especially if you have a condition called hiatal hernia. The question is, what to expect after GERD surgery or endoscopic intervention? Can surgery/endoscopic treatments cure GERD permanently?
Generally, long term observational studies report that 90 to 95% of adults are satisfied with the results of their anti-reflux surgery (ref), (ref).
However, the term “satisfied” doesn’t always mean “cure” as a considerable subset of people may need some anti-reflux medications after surgery. And even about 5 to 10% may need to repeat surgery later (ref).
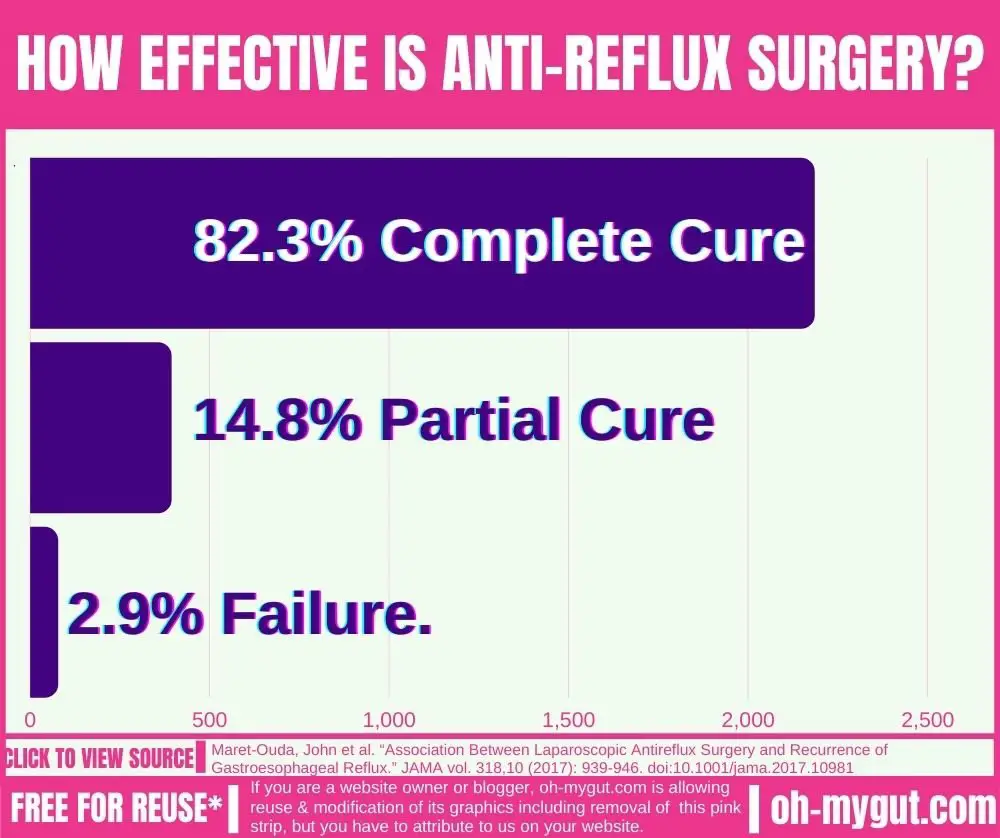
In a large Swedish study of 2655 patients who underwent anti-reflux surgery, 82.3% were permanently cured of GERD, while 17.3% were found to have recurrent GERD symptoms after surgery.
A further follow up of the 17.3% patients (number=470) was done. And found that out of the 470, 16.4% (77 patients) repeated the reflux surgery.
What does this mean?
This tells us that anti-reflux surgeries [in certain cases], can help provide a permanent cure for your GERD. but it depends on multiple factors such as:
- The severity of your GERD.
- Other risk factors such as obesity, older age, co-existing diseases (ref).
- The type of operation.
- Other lifestyle and dietary factors.
MORE:
- 7 Hiatal Hernia Weird Symptoms.
- 7 Effective Hiatal Hernia Pain Relief Tips.