Does Throwing Up Make Acid Reflux Better? A Gut Doctor’s Answer.
Quick Insights:
- There is no scientific evidence that spontaneous or self-induced throwing up can make your acid reflux symptoms better.
- Moreover, it can result in worsening symptoms of GERD or complications in the long term.
- Frequent throwing up leads to more acid and Pepsin enzyme exposure.
- Frequent throwing up may lead to more weakness in your LES. Also, it can lead to a worsening of the hiatus hernia.
- Relief of acid reflux by throwing up may be a transient feeling or reflect another overlooked medical condition such as gastroparesis.
- Work with your doctor to determine the best option that can make your acid reflux better.
The Short Answer: Does Throwing Up Makes Acid Reflux Better?
There is no scientific evidence that spontaneous or self-induced throwing up can make your acid reflux symptoms better. Moreover, it can result in worsening symptoms of GERD or complications in the long term.
Throwing up can be a symptom of severe gastroesophageal reflux disease (especially with hiatus hernia). Or a reflection of co-existing diseases such as gastroparesis.
If you practice self-induced throwing up, you may need to stop and seek medical help from your doctor to avoid further damage or worsening of your condition.
Frequent throwing up leads to more acid and Pepsin enzyme exposure, which can lead to increased frequency of GERD attacks and, subsequently, more complications [ref].
Throwing up to make your acid reflux symptoms better is probably a bad idea in the long term. And we will explain to you why in the next section.
Why Throwing Up Is A Bad Idea For Your Gerd/Acid Reflux?
As we explained before, No clinical or scientific evidence supports that throwing up can make your acid reflux better.
On the other hand, frequent or self-inducing throwing up can negatively impact your GERD in many ways:
1- More Acid/Pepsin Exposure To Your Esophagus.
Throwing up (especially if frequent) will expose your esophagus more to the acid and another enzyme called “pepsin.” Pepsin can break down protein, and your esophagus lining is not an exception [ref].
This esophageal exposure (although transient) introduces larger amounts of harmful stomach contents, which can worsen the already existing esophagitis.
This leads to persistent symptoms and the development of erosions and complications (discussed later).
2- Negatively Affect Your Lower Esophageal Sphincter And Hiatus Hernia.
The principal mechanism of GERD is the weakening of the lower esophageal sphincter (LES). And, in a significant part of patients, it may be due to a condition called hiatus hernia. A hiatus hernia occurs when the upper part of your stomach (including LES) bulges into your chest through the opening (hiatus) in the diaphragm.
In the long term, frequent throwing up may lead to more weakness in your LES. it also can lead to worsening of the hiatus hernia. And after some time, you may start to experience more severe and frequent attacks of GERD flare-ups.
3- Affects Your Throat, Oral Cavity, and Lungs.
Throwing up to relieve GERD can also cause more acid to expose to your throat and oral cavity. And this will have many negative effects [ref]:
- Throat: recurrent or chronic inflammation (laryngitis), sore throat, choking sensations, and cough.
- Teeth: you will experience more dental enamels and gum problems on repeated exposure to the vomitus containing acid.
- Oral cavity: bad mouth odor.
- Lungs and airways: frequent throwing up can lead to aspiration of a part of the vomitus into the airways leading to aspiration pneumonia and reflux asthma. The risk of aspiration is higher due to the passage of a large amount of vomitus at once.
4- Throwing Up Can Lead To Tears In The Lining Of Your Esophagus.
“Mallory-Weiss syndrome” is a famous complication of forceful vomiting. As you throw up, a small tear in the inner lining of your esophagus (the mucosa) can develop. Subsequently, the tear can bleed and that is one of the common causes of experiencing small amounts of bright red blood with vomiting.
Furthermore, with acid reflux, the odds of the development of “Mallory-Weiss syndrome” can be higher due to pre-existing inflamed mucosal lining of the esophagus due to GERD.
5- You Will Be More Likely To Develop GERD Complications.
Frequent throwing up and exposure to larger amounts of acid can raise the odds of developing GERD complications:
- Erosive oesophagitis: inflammation of the lining of your esophagus, which is associated with the breakdown of the inner layer of the esophagus (the mucosa).
- Barrett’s esophagus: the lining cells of your esophagus can gradually transform into another type of cell (like the type lining your small intestine). The development of Barrett’s esophagus is associated with an increased risk of esophageal cancer.
- Esophageal stricture: healing of the inflammation and the erosions can result in fibrosis that leads to the narrowing of the esophagus. Esophageal stricture and narrowing leas to difficulty swallowing (dysphagia).
6- It can lead to the failure of your anti-reflux surgery.
It is known that any straining on your diaphragm and abdominal muscles can lead to the failure of the anti-reflux surgery.
Activities like weight lifting, coughing, sneezing, and ultimately frequent throwing up can weaken the fundoplication operation.
If you have a previous anti-reflux surgery and throwing up, seek help from your doctor or surgeon.
But, When I throw up, My acid reflux becomes relieved?!
It is possible for some people with GERD to feel better after throwing up. But this is either a short-living relief and is usually due to a full stomach as a result of binge eating or drinking.
Also, getting relieved by vomiting should raise the question: is it GERD or maybe something else?
Improvement after throwing up may also indicate another overlooked condition called “gastroparesis.”
Gastroparesis occurs when your stomach loses its spontaneous movement that helps its emptying. And as a result, the food stays longer inside your stomach and triggers symptoms including:
- Nausea after eating for a long time.
- Bloating.
- Loss of appetite.
- Acid reflux symptoms (heartburn).
- Throwing up (which can relieve nausea and bloating).
Your doctor suspects gastroparesis with acid reflux if your symptoms don’t improve with the standard GERD treatments.
Other risk factors of gastroparesis:
- Having diabetes mellitus.
- Taking certain high blood pressure medications.
- Taking medications that slow the emptying of your stomach, such as narcotics.
- Hypofunction of your thyroid gland (hypothyroidism).
- Certain diseases such as scleroderma and parkinsonism.
When your doctor suspects gastroparesis, he will request a specific test called “gastric emptying study” or “scintigraphy”.
Gastroparesis is a not uncommon condition and is often overlooked by both doctors and patients.
What Works For Your Acid Reflux Relief?
We concluded that both spontaneous and self-induced throwing up might be a bad idea for your acid reflux. And it can harm your GERD and cause complications.
So.
In terms of relieving acid reflux, what works?
The answer greatly depends on individual situations, such as the presence of obesity or hiatal hernia (the main factor contributing to your GERD).
Here are evidence-based tips that proved to have more impact in making your acid reflux better:
Lose weight (if you’re obese).
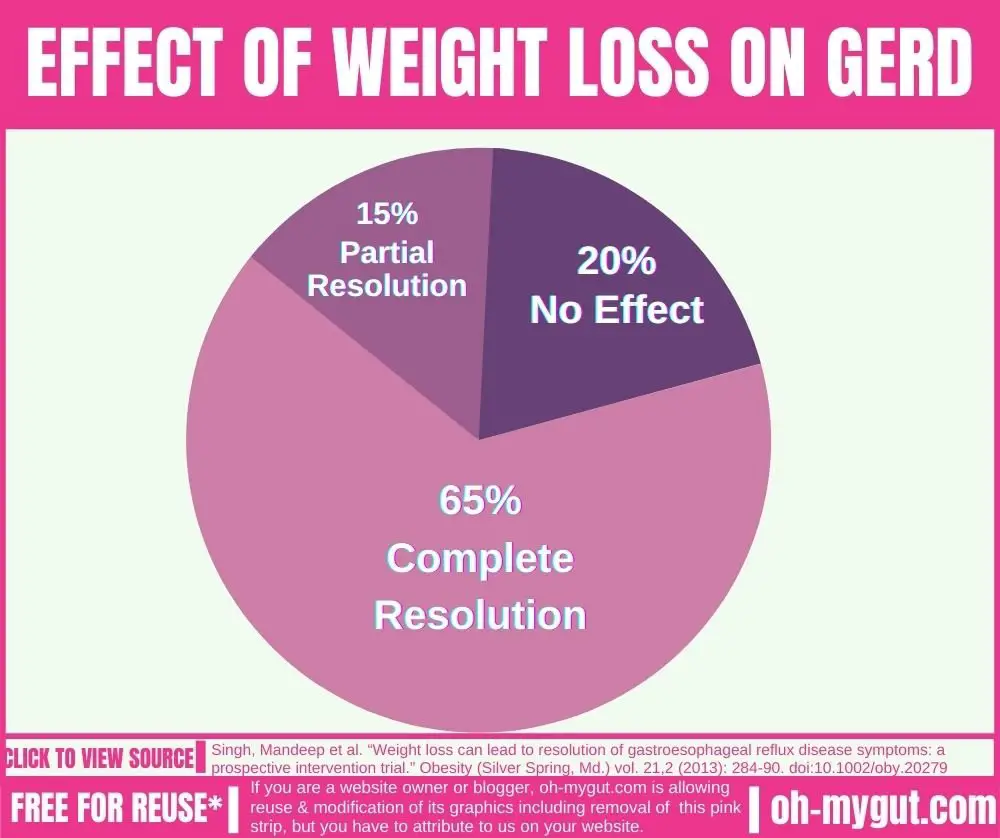
Weight loss (in obese GERD patients) is consistently linked to a major improvement in GERD and acid reflux. Losing weight resulted in a permanent cure for GERD in 65% of obese patients. Another 15% of obese GERD patients experienced partial resolution of GERD [ref].
It appears that losing weight is one of the most effective strategies in relieving acid reflux. Try a weight loss program if you are obese.
Elevate your head & chest during sleep.
Another effective strategy that can lead to significant improvement of GERD is head elevation during sleep. And this includes the elevation of your entire chest and head [ref].
This prevents nighttime reflux and greatly improves GERD symptoms and protects your esophagus, throat, airways from the harmful effect of acid reflux which is great during supine sleep.
It is better to use wedge pillows instead of standard pillows. This is because it does a better job in terms of elevating both your head and chest.
The role of food.
No food can directly improve GERD symptoms. However, avoiding food triggers can prevent acid reflux flare-ups.
The most important foods to avoid are caffeine, fatty foods, spicy foods, and tomatoes. Also, avoiding large meals and nighttime meals 3-4 hours before sleep can help [ref].
PRO TIP: You can use food strategically to relieve your acid reflux by sticking to a weight loss diet program.
The role of medications.
Although medications cannot cure GERD permanently, it has an important role in controlling symptoms and preventing complication and damage to your esophagus [ref].
Use medications as guided by your doctor as there is no food or alternative remedy as effective as medications in controlling your acid reflux.
Work with your doctor.
If you experience severe GERD symptoms, frequent vomiting, or hiatus hernia, discuss the issue with your doctor to determine the best solution to make your acid reflux better.
An effective option for severe or refractory forms of acid reflux is anti-reflux surgery. Working with your doctor can help determine the best option for you.
MORE: Can you Throw up from not Eating All-day?







