6 Causes of Brown, Coffee-Ground Vomiting On Empty Stomach.
Our content is not intended nor recommended as a substitute for medical advice by your doctor. Use for informational purposes only.
Dark brown or coffee-ground vomiting on an empty stomach is often caused by minor bleeding from the stomach, esophagus, or duodenum.
The most common causes of coffee ground vomiting on an empty stomach include gastritis, esophagitis, peptic ulcer disease, GERD, and intestinal obstruction.
Although coffee-ground vomiting is not as life-threatening as frank bloody vomiting (hematemesis), it is considered an emergency and should be managed immediately by your doctor.
This article will dive into the most common causes of coffee ground vomiting on an empty stomach, its risk factors, and its symptoms.
1. Gastritis or duodenitis.
Inflammation of your stomach or duodenum lining is called gastritis/duodenitis.
It is caused by several conditions and risk factors, most commonly (reference):
- H. pylori infection ( a bacteria that infects your stomach and leads to gastritis or ulcers).
- Medication abuse: most commonly, Nonsteroidal anti-inflammatory drugs (such as ibuprofen and ketorolac).
- Excessive alcohol consumption.
- Chronic psychological stress.
- Bile reflux.
- Smoking.
- Faulty diet habits (excess caffeine, spicy, fried, and fatty foods).
Mild gastritis or duodenitis typically doesn’t bleed. However, it may cause coffee ground (brown or blackish-brown) vomiting if the inflammation is severe (due to small erosions in the mucosal lining).
The coffee ground vomit occurs due to oozing blood from the severely inflamed mucosal lining of the stomach/duodenum.
The bleeding from gastritis or duodenitis is typically minimal in amount. Stomach acid breaks this small amount, blood-forming an acid-hematin mixture that is coffee-ground-like.
Symptoms:
- Burning or gnawing pain or discomfort in your abdomen’s upper central (epigastric) area.
- The pain is often chronic or recurrent with periods of exacerbations.
- The pain often occurs after eating heavy, fatty meals and drinking caffeine, alcohol, or spicy foods.
- Nausea.
- The bleeding from gastritis or duodenitis is often minimal, leading to vomiting of coffee ground fluid (especially if your stomach is empty).
- Rarely the bleeding becomes significant (moderate to severe), leading to vomiting of clotted blood or passing clear stool.
- Anorexia (loss of appetite).
- Recurrent fullness or discomfort in the epigastric area (bloating).
- Difficult digestion (dyspepsia).
How Gastritis/duodenitis is diagnosed?
Your doctor considers gastritis a cause of coffee grounds or brown vomiting when you have a typical history of recurrent dyspepsia (indigestion).
To confirm the diagnosis, your doctor will need an upper gastrointestinal endoscopy to visualize the inflammations and define the bleeding source.
Also, your doctor may order tests (blood, stool, or urea breath test) to define the cause, such as H. pylori testing.
2. Peptic ulcer disease.
Peptic ulcer disease often occurs due to the same causes or risk factors as gastritis.
A peptic ulcer is a breakdown (sore) in the lining of either:
- The stomach (gastric peptic ulcer), Or
- The duodenum (duodenal peptic ulcer).
Peptic ulcer bleeding is typically moderate to severe. So, bleeding peptic ulcers often present with frank vomiting of dark or bright red blood (not coffee ground).
However, small ulcers may cause minor bleeding, which leads to brown or brown-black, coffee-ground vomiting on an empty stomach.
Symptoms of peptic ulcer disease.
- Many peptic ulcers are asymptomatic (reference).
- Gastritis-like symptoms (epigastric pain, dyspepsia, nausea, vomiting, and anorexia).
- Minor bleeding leads to coffee ground vomiting (especially on an empty stomach).
- Moderate to severe bleeding leads to vomiting of frank blood (red or dark red and clotted blood) and melena (black tarry stool).
- Signs of shock often occur with severe bleeding, such as shortness of breath, fast heartbeats, dizziness, lightheadedness, confusion, fainting, or even coma.
- acute and chronic gastric ulcers can block the passage of food from the stomach by causing pyloric stenosis in adults. This can lead to a condition called gastric outlet obstruction which can lead to vomiting.
The table below summarizes the differences between gastric and duodenal peptic ulcers.
| Duodenal Ulcer | Gastric Ulcer |
|---|---|
| The primary pain is in the epigastric area and may spread to the left or right hypochondrium and the back. | The same pain locations and radiations. |
| Often improved by eating. | Often aggravated by eating. |
| Good appetite, with normal or overweight. | Loss of appetite is often associated with weight loss. |
| Pain starts later after eating (two to four hours after meals). | Pain starts shortly after eating (within one to two hours) |
| The pain is often episodic (short-lived attack sort-lived). | The pain is often persistent for long hours or days. |
| More likely to occur at night (up to 88% of the time). | Less common for the pain to occur at night (up to 48%). |
| Nausea and vomiting are slightly less common | Nausea and vomiting are slightly more common |
| Less likely to turn malignant | More likely to turn malignant (gastric cancer), especially in the elderly. |
| Associated with H. Pylori infection100% of the time. | Associated with H. Pylori infection 70% of the time |
| When it bleeds, it is more likely to cause hematemesis (vomiting of blood which is often coffee-ground or red). | It is more likely to cause melena (black stool) when it bleeds. |
Endoscopy is the gold standard for diagnosing peptic ulcers or any cause of vomiting blood or coffee-ground material.
MORE: Throwing Up Stomach Acid: 3 Main Causes & Treatments.
3. Esophagitis.
Esophagitis (inflammation of the esophageal lining) is another very common condition affecting patients with acid reflux (GERD) and other diseases.
Esophageal erosions due to severe esophagitis cause minor bleeding that reaches the stomach. The blood turns into a coffee-ground, black or brown fluid in the stomach when it mixes with the stomach acid and digestive enzymes.
The coffee-ground fluid can be vomited when the stomach is empty, leading to brown or brownish-black fluid in the vomit.
Causes of esophagitis:
- GERD (gastroesophageal reflux disease) or chronic acid reflux is the COMMONEST cause of esophagitis.
- Medications (pill esophagitis): such as erythromycin, tetracycline, clindamycin, NSAIDs, potassium chloride, oral bisphosphonates, and iron supplements.
- Infections: Herpes simplex virus (HSV), Cytomegalovirus (CMV), Candida albicans, HIV, etc. (affects patients with a weak immune system).
- Others such as lymphocytic and eosinophilic esophagitis.
The image below is taken from an endoscopy camera inside the esophagus. Notice the erosions and redness resulting from the severe inflammation of the esophageal lining.
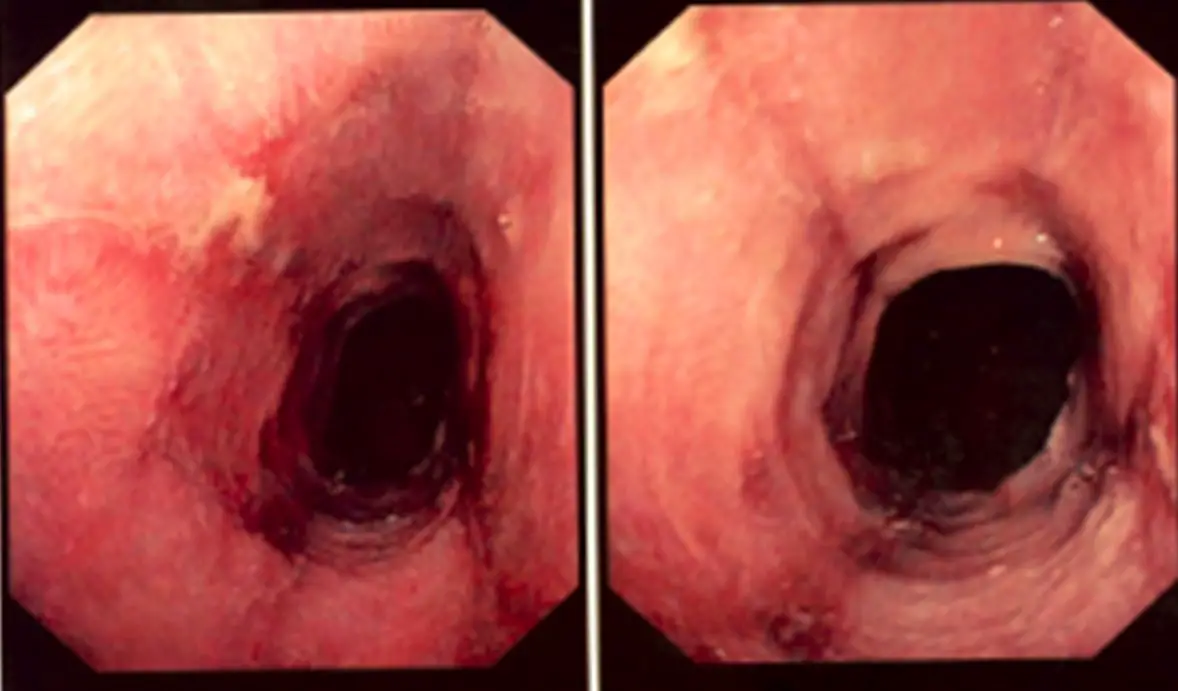
Symptoms of esophagitis (Acid reflux):
- Chronic or recurrent heartburn (burning sensation in the chest).
- Regurgitation of food or acidic fluids into the throat.
- Difficulty swallowing.
- Sore throat, dental caries, bad mouth odor (due to acid reflux to the mouth & throat).
- Chronic cough, asthma, and shortness of breath (due to acid reflux to the respiratory airways).
- Nausea.
- Vomiting: severe esophagitis can cause coffee-ground vomiting when bleeding from the inflamed mucosa occurs.
- Chocking attacks during the nighttime.
- Globus sensation.
4. Nose, mouth, or throat bleeds (False hematemesis).
Doctors use “false hematemesis” in medical practice to describe the vomiting of previously swallowed blood.
You may swallow blood from your nose, mouth, or throat to your stomach. Eventually, the blood is digested by your stomach acid to form a coffee-ground acid hematin which can be vomited again on an empty stomach.
Common causes of swallowing blood include:
- Gum bleeding.
- Nose bleeding (from the posterior part of the nose).
- Post-tonsillectomy bleeding.
- Tooth extraction.
- Bleeding mouth or throat ulcers or severe infections.
The bleeding from your nose, mouth, or throat is often visible. However, some patients may not notice the bleeding event (as in children, the elderly, and patients with mental disabilities).
People who swallow blood and vomit it again as coffee-ground brown fluid often don’t have symptoms (such as epigastric pain, dyspepsia, etc.).
Report any bleeding events to your doctor (mouth, nose, throat) bleeds if you have coffee-ground vomiting on an empty stomach.
5. Stomach or esophageal cancer.
Patients with cancer in the esophagus or stomach may have coffee-ground or brown vomiting (on an empty stomach). In addition, the malignant tumor in the esophagus or stomach may ulcerate and cause minor bleeding.
The suspicion of the stomach and esophageal cancer depends on:
- The presence of risk factors.
- The characteristic clinical features.
A. Esophageal cancer.
Esophageal cancer is the 8th most common cancer and the 6th-most common cause of cancer death worldwide (reference).
Risk factors:
- Smoking.
- Alcohol abuse.
- Spicy foods.
- Chronic acid reflux (gastroesophageal reflux disease).
- Bile reflux.
- Difficulty swallowing (achalasia).
- Habitual drinking of very hot liquids.
- Lack of eating enough fruits or vegetables.
- Selenium deficiency.
- Obesity.
Symptoms:
- Difficulty swallowing (dysphagia) that worsens over time.
- Progressive weight loss without trying.
- Heartburn or chest pain.
- Chronic indigestion.
- Nausea.
- Vomiting (can be coffee-ground in color) if the mass is bleeding.
- Hereditary and genetic factors.
B. Stomach cancer.
Risk factors:
- H. pylori infection.
- Being older.
- Family history of stomach cancer.
- High-salt diet (as salt-preserved food).
- Smoking and alcohol.
- Long-term gastrirtits.
- Stomach polyps.
- Obesity.
- N-nitroso compounds are found in food (cheese, fish, bacon, and other cured meat.
- N-nitroso compounds in other sources, such as beer, tobacco smoke, and chewing tobacco.
- Radiation exposure.
Symptoms:
- Difficulty swallowing (dysphagia).
- Persistent bloating and early satiety.
- constant indigestion (dyspepsia).
- Weight loss without trying.
- Nausea.
- Recurrent vomiting (food, stomach acid, or coffee-ground vomiting).
- The vomiting can occur on an empty stomach if the mass is large or causes inflammation.
- Persistent stomach pain (usually, doesn’t respond to ant-acid treatment).
- Passage of black stool (melena).
6. Intestinal obstruction.
Patients with intestinal obstruction may suffer from large-volume, coffee-ground vomiting even if they are fasting.
Coffee ground vomiting on an empty stomach can be stomach contents (or even fecal matter) rather than blood in patients with intestinal obstruction.
Common causes of intestinal obstruction include:
- Intestinal or colon cancers.
- Strictures (narrowing), as in patients with Crohn’s disease.
- Intraabdominal adhesions (common among patients who have previous multiple abdominal operations).
- Twisting of the intestine around itself (volvulus).
- Congenital intestinal obstruction in newborns.
- Foreign bodies.
- Gallstone obstructing the small intestine (gallstone ileus).
Symptoms:
- Absolute constipation.
- Inability to pass flatus.
- Abdominal pain (cramps).
- Severe bloating and distension.
- Vomiting of fecal material, bile, or coffee-ground material.
- Loss of appetite (nausea).
7. Other causes.
Other less common causes of coffee-ground or dark brown vomiting on an empty stomach include:
- Medications such as nonsteroidal anti-inflammatory drugs and some antibiotics.
- Esophageal or stomach varices in patients with end-stage liver disease (liver cirrhosis).
- Portal hypertensive gastropathy (severe congestion in the stomach lining due to diseases causing portal hypertension as cirrhosis).
- Vascular malformations (angiodysplasia) include Dieulafoy lesions and gastric antral vascular ectasia.
- Cameron lesions (linear ulcers that bleed in the upper part of the stomach in patients with hiatal hernia and GERD).
- Post-operative bleeding in patients with stomach, esophageal, or duodenal operations.
- Bleeding from the biliary system (haemobilia).
- Bleeding from the pancreas (Hemosuccus pancreatic).
- Evidence-based
- Written by a doctor.

















