How To Diagnose IBS (Simplified + Quiz), Doctor Explains.
Our content is not intended nor recommended as a substitute for medical advice by your doctor. Use for informational purposes only.
Navigating the realm of medical conditions can be a daunting task, but that’s why I’m here to help. If you stick with me and read through this article, you’ll stand a 95% chance of accurately identifying whether you’re dealing with Irritable Bowel Syndrome (IBS). Please keep your eyes peeled for the detailed symptoms we’ll cover, which could be the key to determining your gut issues.
ibs-diagnosis-made-simple
Hello, I’m Dr. Islam, a seasoned gastroenterologist. I’m about to break down the process of diagnosing IBS for you.
Let’s get one thing straight…
This article doesn’t replace a consultation with your doctor. Instead, view it as a stepping stone towards solving the digestive problems plaguing you.

How To Diagnose IBS
Here’s the kicker – we don’t have a test to diagnose IBS definitively. IBS is categorized as a “functional” disorder, meaning we – the medical practitioners – can’t pinpoint any specific lesion or disease within your gut causing the symptoms.
However, don’t lose heart. You can try to diagnose IBS by using the ROME IV criteria. This tool was developed to assist doctors in diagnosing IBS, and it can be handy for you, too, especially if you suspect IBS (reference).
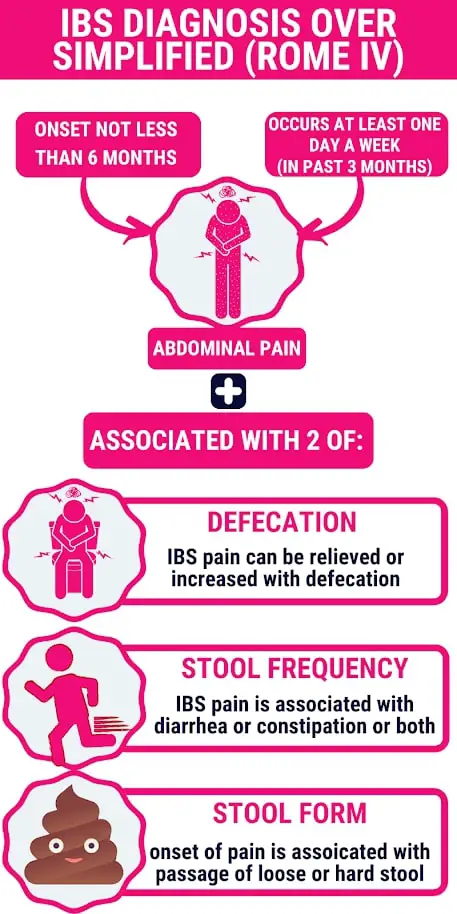
The Rome IV criteria can be applied as follows:
Applying the Rome IV criteria is simple:
In layperson’s terms, you might be dealing with IBS if you’ve experienced:
Your initial episode of abdominal pain lasted for six or more months. You’ve had abdominal pain on at least 3 days every month in the past 3 months. Your abdominal pain tends to improve or worsen after you defecate. Your stool frequency fluctuates with episodes of abdominal pain (you either have constipation or diarrhea). Your abdominal pain episodes are accompanied by a change in the appearance of your stool.
You need to have both (1) & (2) and any two of (3), (4), & (5).
Or you can take THIS QUIZ (from doctoroz.com) if you feel confused.
But…
Remember to consult your doctor about your digestive concerns. They can review your symptoms and perform some tests if necessary to rule out other conditions before diagnosing you with IBS.
How IBS symptoms exactly look like?
To make it clear for you, I will exactly describe every symptom of IBS.
1- Abdominal pain or discomfort.
The gut cramps related to IBS are typically described as colicky (painful contractions followed by periods of relaxation in your gut). It’s not a constant pain.
IBS pain isn’t restricted to your upper abdomen (epigastric area), but it can occur anywhere in your abdomen, especially in the lower part.
The pain tends to intensify during your working hours, after meals, and often more in the mornings. Conversely, it lessens while you’re asleep.
The distress of IBS usually flares up with emotional stress. You may also feel a sense of bloating, fullness, or excess gas in your abdomen.
2- The pain is related to defecation.
Most IBS patients report relief of abdominal pain after passing stools.
However, some report the opposite – the pain worsens after defecation. Either way, this correlation between abdominal discomfort and defecation is a useful clue in diagnosing IBS.
3- Irritable bowel syndrome with predominant diarrhea (IBS-D). How it exactly looks?
You may be dealing with IBS-D if your stools are typically loose during flare-ups (more than 25% of bowel movements involve diarrhea). The passage of loose stools usually happens in the morning, during working hours, or post meals.
The loose stools are usually small or moderate in volume.
If you have a sudden passage of large volumes of loose stools, it’s probably an infection, not IBS-D.
You might also experience lower abdominal cramps before a diarrhea episode and feel complete evacuation afterwards.
Passing mucus with stool during an IBS-D flare-up is quite common, as reported by 50% of individuals with IBS-D.
However, if you notice blood in your stool, experience diarrheal episodes during sleep, or have a fever with diarrhea, you should immediately seek medical help.
4- Irritable bowel syndrome with predominant constipation (IBS-C). How it exactly looks?
You may have IBS-C when your stools are usually hard and difficult to pass (in more than 25% of your bowel movements).
People with IBS-C often experience “tenesmus,” which is a feeling of incomplete evacuation or difficulty in passing stool, even after defecation.
It’s important to note that having constipation without abdominal pain does not equate to IBS-C but rather signifies “Chronic Constipation.”
5- Irritable bowel syndrome: the mixed (IBS-M) and unclassified (IBS-U) types.
The mixed type of IBS implies you have a blend of both constipation and diarrhea (constipation more than 25% of the time and diarrhea more than 25% of the time).
The unclassified type of IBS refers to the presence of abdominal pain without a specific dominance of either constipation or diarrhea.
Why & When You Should Consult Your Doctor
If you haven’t been diagnosed with IBS before, it’s crucial to consult your doctor. They will gather a detailed history and perform an examination.
Your doctor will have a better understanding of the nuances of the disease symptoms and can prescribe a suitable treatment.
If you already have IBS, you should consult your doctor if you experience any If you have any of them, consult your doctor immediately. Always notify your doctor if you have a family history of colon cancer or Inflammatory Bowel Disease. You have to know that having IBS is not the end of the world. It is a benign disease and can be controlled. You will not die from IBS and it is not a disease that progresses or leads to other diseases. It is controllable by lifestyle and dietary changes.
Can IBS be misdiagnosed?
Sometimes, IBS gets confused with other diseases. So, be careful of these warning signs. If they appear alongside IBS, there might be a more serious problem.
Watch out for these signs:
1- You start experiencing IBS symptoms after the age of 50:
Typically, IBS starts when you’re younger, often in your 20s or 30s.
Starting to have IBS symptoms after the age of 50 isn’t normal. If you’re 50 or older and have stomach pain, constipation, or diarrhea, go see your doctor right away. They’ll check for other things like colon cancer.
2- You find red or black blood in your stools:
Blood in your stools could mean:
- Red blood: This can come from bleeding in the last part of your colon (anorectum) or from a large amount of bleeding anywhere in the colon. If there’s a lot of blood, it doesn’t stay in the colon long enough to turn black.
- Black blood: When blood stays in the colon long enough, it gets digested and turns black. It then looks like “tar”.
Seeing blood in your stool isn’t normal for IBS. If you notice any blood, go to your doctor right away.
Blood in your stool can mean many things, including benign conditions like piles or dysentery, or more serious conditions like colon or rectal cancer.
If you want to learn more, read this article about IBS and colon cancer.
3- Diarrhea wakes you up at night:
Usually, IBS-caused diarrhea happens in the morning or during work hours, not when you’re sleeping.
If diarrhea is waking you up at night, talk to your doctor to find out why.
4- Your stomach pain is getting worse each day.
IBS stomach pain usually comes and goes. Some days you feel pain, other days you don’t.
If your stomach pain is always there, or it’s getting worse each day, go see your doctor.
5- You’re losing weight quickly.
Certain chronic bowel infections, colorectal cancer, and inflammatory bowel disorders can make you lose a lot of weight. IBS doesn’t.
If you lose more than 10 pounds (4.5 Kg) or more than 5% of your body weight in 6 to 12 months, it’s a lot.
6- Your family has a history of IBD or colorectal cancer.
IBD or Inflammatory Bowel Disorders like Ulcerative colitis and Crohn’s disease cause inflammation in your colon and intestine.
If someone in your family has colon cancer or an inflammatory bowel disorder, you have a higher risk of getting these diseases too. And their symptoms can look a lot like IBS.
So…
If your family has a history of these diseases, let your doctor know.
Your doctor will run some tests to rule out these diseases.
7- You have anemia and don’t know why.
One common cause of unexplained anemia is losing small amounts of blood from your gut over time.
You might not see blood in your stools if you’re losing a small amount. But if it happens every day, you can end up with anemia.
So if you have both anemia and IBS symptoms, tell your doctor.
Common Questions Asked By My Patients; Answered.
Q: How long do IBS attacks last?
A: IBS attacks typically last between 2-4 days. However, this can vary greatly. Some people might only have an attack for a few hours, while others may experience symptoms for over a week.
Q: What does IBS pain feel like?
A: Here’s a brief overview of what IBS pain can feel like:
- It can feel like your intestines are tightening and then relaxing, but it’s not constant.
- The pain can be anywhere in your belly, but many people feel it more in the lower part.
- It often happens during work hours and in the morning, but usually not when you’re asleep.
- Certain foods, like FODMAPs and foods that cause gas, as well as stress, can make the pain worse.
- Going to the bathroom can sometimes help ease the pain, but some people find it makes their pain worse.
Q: Does IBS ever go away?
A: IBS is a long-term condition. It can have times when symptoms get worse and times when they improve.
While IBS can’t be cured, many people manage their symptoms through lifestyle changes, diet, and managing stress. Though it’s not harmful in itself, IBS can seriously impact quality of life.
Q: Can IBS develop suddenly?
A: Yes, IBS can develop suddenly. This usually happens after an intestinal infection (this is called “post-infectious IBS”) or a major stressful event, like the death of a loved one.
Q: How do you test for irritable bowel syndrome?
A: There’s no lab test for IBS. Instead, doctors ask you about your symptoms, like stomach pain, constipation, or diarrhea. They then compare your symptoms to the ROME IV criteria to diagnose IBS.
In some cases, doctors might run tests to rule out other conditions that have similar symptoms to IBS. These tests can include blood tests, stool analysis, tests for celiac disease, or a colonoscopy, where a camera is used to look at your colon.
What can be mistaken for IBS?
Several conditions can have symptoms similar to IBS, including:
- Inflammatory bowel disease (IBD), including Crohn’s disease and ulcerative colitis.
- Celiac disease: an immune reaction to gluten that causes inflammation in the small intestine.
- Lactose or fructose intolerance: some people can’t properly digest these sugars, leading to gastrointestinal symptoms.
- Gastroenteritis: an infection or inflammation of the stomach and intestine.
- Endometriosis: in some women, tissues similar to the lining of the uterus can grow outside of the uterus, sometimes leading to bowel symptoms.
- Colon or ovarian cancer: while these are less common, they can sometimes present with similar symptoms to IBS.
Does IBS show up on a CT scan?
No, IBS doesn’t show up on a CT scan. IBS is a functional disorder, which means it affects how your gut works rather than causing visible changes to the structures of your digestive system. CT scans, like other imaging tests, can help rule out other conditions that might mimic IBS, such as diverticulitis, tumors, or inflammatory bowel disease, but they can’t directly diagnose IBS.
Key messages:
- IBS is diagnosed by matching your symptoms to a specific pattern, not through a specific test.
- You can try to figure out if you have IBS by using the ROME IV criteria or by taking this QUIZ.
- To self-diagnose accurately, you should understand the details of the symptoms mentioned in this post.
- This article isn’t a replacement for a doctor. If you think you have IBS after reading this, make sure you see a doctor.
- Don’t ignore IBS warning signs like blood in your stool, fever, anemia, weight loss, and diarrhea at night.
- Evidence-based
- Written by a doctor.






